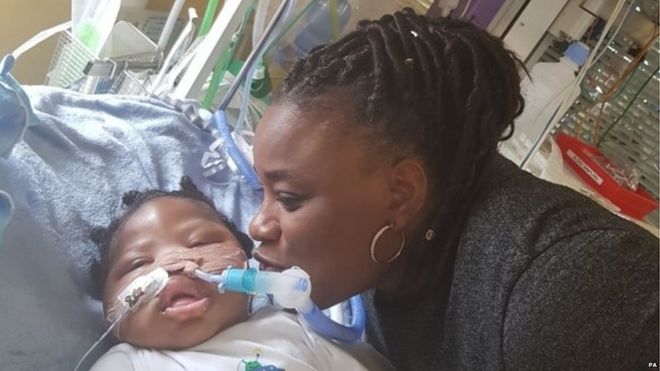
Doctors can stop life-support treatment to a brain-damaged 11-month-old against his parents’ wishes, a High Court judge has said. Isaiah was born with brain damage after a difficult birth during which his brain was starved of oxygen. King’s College Hospital wanted to give only palliative care to Isaiah Haastrup because he needed continuous ventilation and showed no awareness of his surroundings because of his severe brain damage and felt continuing ventilation was “not in his best interests”.
Isaiah’s mother, Takesha Thomas said ‘I see a child who is injured. He needs love. He needs care. I have it. I can give it,” talking about his life she said ”To say it is so poor, it is not worth living, that is not right. It is not their decision to make.”
Parents often believe they have the right to decide what happens to their child. However that is not strictly true in law and according to medical ethics doctors have a duty to do what they think is best for their patient, the child. If it is an emergency they may treat the patient against the wishes of a parent for example. When ever possible if there is time however they will make a child a ‘ward of court’ and a judge will decide.
Barrister Fiona Paterson, representing King’s College Hospital NHS Foundation Trust, said nobody could understand the pain and suffering Isaiah’s parents had endured. However, she said overwhelming medical evidence showed stopping treatment was best for Isaiah.
Mr Justice MacDonald said he passed his ruling that Isaiah’s life support should be switched off with “profound sadness”.
Children and consent;This case raises ethical issues of consent and autonomy. Adults have autonomy and the right to make bad decisions for themselves. Steve Jobs of Apple refused to have surgery for his pancreatic cancer when it was first diagnosed, preferring macrobiotics and positive thinking despite the pleas from his doctors and family to have the standard conventional treatment [he later fully embraced what ever medicine could offer him and underwent two liver transplants]. Seven year old children do not have autonomy so usually their parents are regarded as being guardians of their best interests. However when this seems not to be the case, doctors/hospitals can apply to court and the child can be made a ‘ward of court’ and decide what is in the child’s best interest. The court has to decide what would be in the child’s best general interest not necessarily the child’s medical best interest. So this is usually only done for severe life threatening illnesses. For example I know of a case of a Jehovah‘s witness boy who was recommended a blood transfusion but whose parents refused it. The boy was instead given iron injections [which are notoriously painful] over several months because although a transfusion was in the boy’s medical best interest it was thought that this would endanger how his parents felt about him and injections would be in his overall best interest.

